Strengthen the Workforce & Enhance Rural Sustainability
The Need
The direct care workforce is the backbone of the HCBS system. These frontline workers enable members to remain living safely in their homes and communities. Unfortunately, pre-COVID workforce shortages have been further exacerbated by the impacts of the pandemic as well as the increase in demand for HCBS services. Additionally, our direct care workforce has served on the frontline, risking their health and safety to ensure our members maintain theirs.
Recruitment and turnover among frontline staff are the most frequently reported provider challenges. Provider recovery payments and wage pass-throughs will provide short-term relief to ensure provider solvency and a wage increase to both reward and retain committed direct-care staff. This will be done in a reasonable ratio and in complement to longer-term, transformational strategies. Incentives to these workers to both thank them for their commitment throughout the pandemic and to recruit and retain them into the future, are also important rewards that will help strengthen and grow the workforce. In addition to direct payments to workers, enhancing the system to better train, support, and advance direct care workers, will ensure higher quality services are delivered resulting in better health outcomes for members. The capacity of the provider network, particularly in rural communities, is thin - driven by the limited workforce availability, difficult economic conditions, and long distances that must be traveled to serve community-based members. Investments in the workforce to expand recruitment and improve retention will bolster both provider capacity and members’ quality of care. A particular emphasis on rural provider sustainability will be made to ensure access to care across the state.
Initiative 1.01. - Increase Payments to Providers and Workers
Read a more in-depth summary of this project's outcomes

Initiative 1.02. - Direct Care Workforce Data Infrastructure
Read a more in-depth summary of this project's outcomes

Initiative 1.03. - Standardized Core Curriculum & Specialization
Read a more in-depth summary of this project's outcomes

Initiative 1.04. - Resource and Job Hub
Read a more in-depth summary of this project's outcomes

Initiative 1.05. - HCBS Workforce Training Fund
Read a more in-depth summary of this project's outcomes

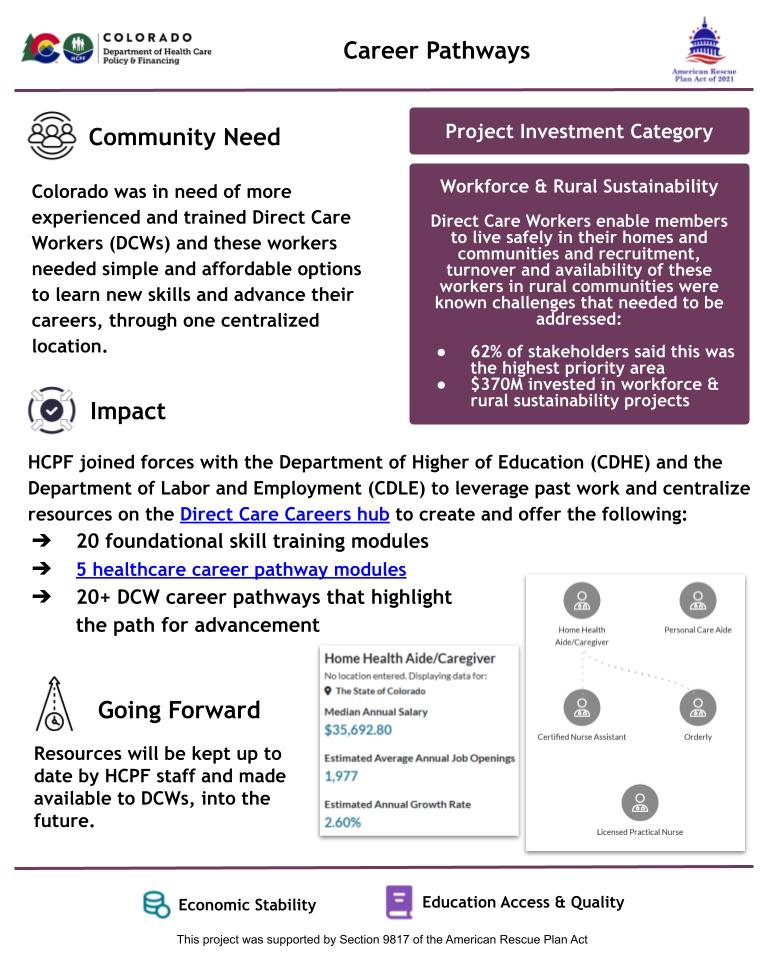
Initiative 1.06. - Career Pathways
Read a more in-depth summary of this project's outcomes
Initiative 1.07. - Public Awareness Campaign
Read a more in-depth summary of this project's outcomes
Initiative 1.08. - Home Health Delegation
Read a more in-depth summary of this project's outcomes

Initiative 1.09. - Workforce Compensation Research
Read a more in-depth summary of this project's outcomes

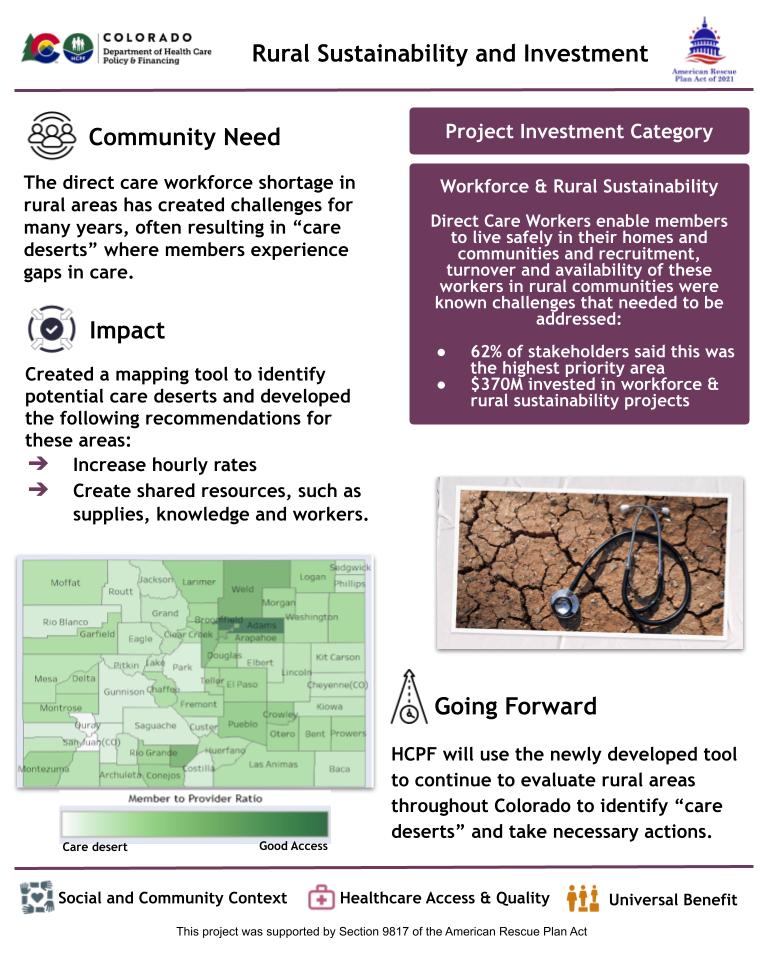
Initiative 1.10. - Rural Sustainability and Investment
Read a more in-depth summary of this project's outcomes